I wouldn’t put any money on the accuracy of my memory as to the attitude of Alexander Langmuir about Tuskegee. What I think I remember distinctly is that the Tuskegee Syphilis Study was briefly mentioned and discussed in the Epidemic Intelligence Service course I audited in the summer of 1957at the CDC. It was discussed as if it were an ordinary investigation to discover more about the natural course of syphilis.
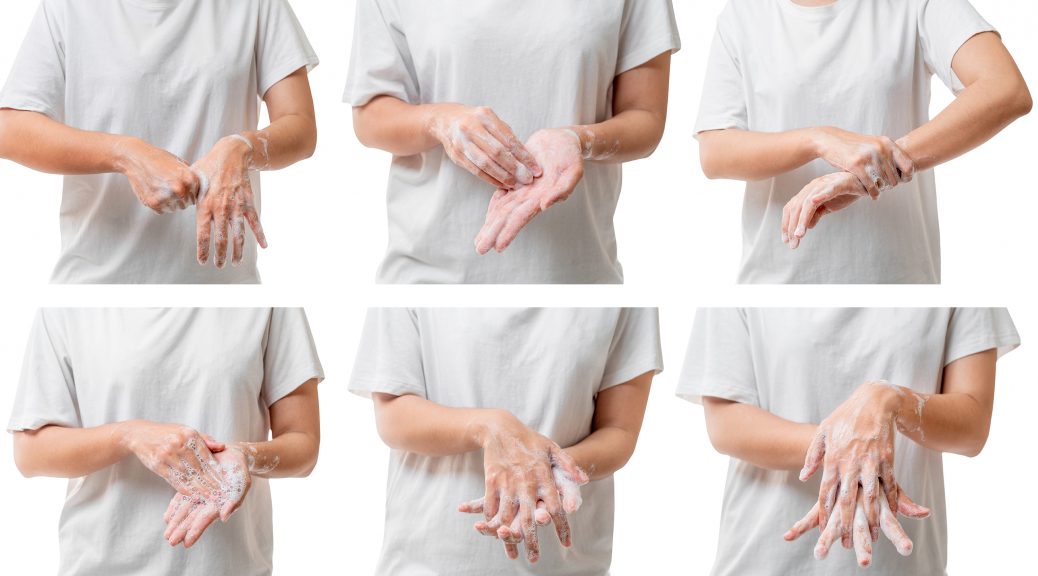
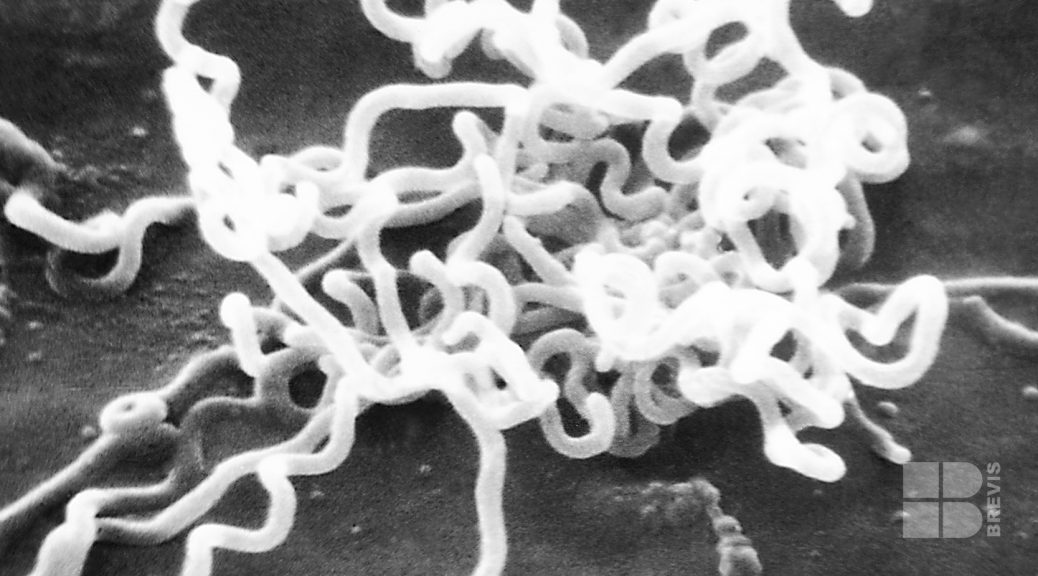
Syphilis, the Great Imitator, has 4 phases: Primary (chancre), Secondary (rash– the Great Pox), Latent, and Tertiary. Each has its own unique characteristics that help to make syphilis “The Great Imitator.” Treponema pallidum, the causative agent is a sneaky devil that can go underground for decades clinically while eating away at vital organs. In 1932, when the Tuskegee Study began, there was considerable uncertainty about many aspects of the natural history of this disease. For example, when syphilis enters its latent stage, is it inevitably going to end in tertiary syphilis with aortic aneurysms or general paresis of the insane or tabes dorsalis or gummas? Or might there be a spontaneous cure? And what is a “cure”? A negative Wassermann test (which was known to be unreliable at that time)? Since the latent phase could last for several decades, there would be a good chance that the patient would die of some unrelated condition such as stroke or heart attack. So what effect would syphilis have on life expectancy?
Visit Brevis.com
In 1930 there was considerable speculation about these questions and so it seemed desirable to study the disease prospectively over an extended period of time. And so the Tuskegee Syphilis Study was begun in 1932. But why Tuskegee and who were the subjects?
It had been observed that in Macon county, home of the famous Tuskegee Institute founded by Booker T. Washington, about 35% of the male, Negro population had a positive Wassermann test for syphilis. (About 80% of the Macon County population was black.) These men were mostly sharecroppers, many illiterate. They were poor and unlikely to be able to afford antisyphilitic therapy. Therefore this population represented a group that could be observed for an extended period without ethical concerns about “doing no harm” since they weren’t going to be able to afford treatment anyway.
Incidentally, the study was later heavily criticized because the subjects were treated as “guinea pigs” and not as humans. But may I remind any gentle readers that Negro slaves were defined in the US Constitution (Article 1, Section 2) as 3/5 of a white person. Negro slaves were further defined as “property” and could not become citizens (See Dred Scott decision and Roger Taney , Chief Justice of the US Supreme Court). Thank you, Founding Fathers (who were mostly slave-owning southerners). Not guinea pigs but maybe like upright beasts of burden. This attitude did not disappear immediately after the Emancipation Proclamation.
The plan was to recruit about 400 men with a positive Wassermann who were in the latent, asymptomatic phase. Those who were in the early stage, roughly five years after the primary chancre, would be referred for treatment and were not eligible for the study. About 200 men with negative Wassermanns would be recruited as controls. But what does it mean to “observe”? The patients had to be given physical exams periodically and also have repeat Wassermanns and spinal fluid exams to look for neurological changes. That’s heavy-handed “observation.”
The study has been criticized because the subjects were not treated with a full course of the prevailing antisyphilitic drugs. (They were treated with a suboptimal course of several months.) But before the late forties when penicillin became the accepted treatment, the standard treatment was the arsenicals, arsphenamine or neoarsphenamine. These treatments consisted of painful intramuscular injections administered monthly for at least a year. All aside from the possibility of a Jarisch-Herxheimer reaction, an asymptomatic patient had a right to to question this procedure. Furthermore, from a medical perspective it was unclear as to the effectiveness of treatment at this stage of the disease and what benefit might ensue. The youngest subjects recruited in 1932 were age 25. By 1948 the subjects were then at least 41 and most were older. At this point the ethical situation begins to become murky. Would treatment be beneficial? But there was much uncertainty and that is why the study was being done. There was considerable incentive to continue as before.
In studies such as this, the investigators have been criticized for treating the subjects as guinea pigs and not as human beings. How could this be so if the study was utilizing some black doctors and the Tuskegee Institute and the indomitable black nurse, Nurse Rivers?
I got some insight into this by my experience living in the South, first from February 1942 to June 1943 on Parris Island, the Marine boot training camp. The top medical officers for the Parris Island base hospital consisted of a Commanding Officer, a Chief of Surgery, an Executive Officer, and a Chief of Medicine (my father). The separate houses were lined up in a row and behind each pair was a maid’s quarters. One weekend when our maid, Lucy, was at her home on the mainland, I looked into these quarters. These consisted of two plain bare rooms each containing a bed and a dresser and bare wooden floor. Between the rooms was a “bathroom” with a sink and toilet. If there was a tub or shower, I didn’t notice it. To the eyes of this 11-year-old kid, raised in an upper middle class suburb of New York, this was a shock, to use a mild expression. But Lucy was always cheerful with nary a complaint. I guess she “knew her place.”
It took me a bit longer to learn mine. One time I had occasion to ride by myself on a public bus some where off the island. At age 11 I wasn’t very tall and when I got on the bus, it looked like every seat was taken. Except that straight down the aisle there was a vacant seat in the middle of the back row. To which I headed.
After I sat down and started looking around, I noticed that all the people sitting around me were highly pigmented and all the palefaces were in the front half. What to do? Nothing that seemed reasonable. So I sat there. The black people around me were too polite to say anything and I was too bashful. But I couldn’t help wondering what they were thinking.
Fifteen years later with a wife and baby son, I returned to the deep South to begin my service as a medical officer with the USPHS in Savannah from August 1957 to August 1959. We attended a small Adventist church, membership about 100, that was on a side street that wasn’t paved. The church itself was clean but definitely showing its age. Not antebellum but certainly not modern. However, we soon fell in love with the members there, all delightful, kind souls. In Savannah at that time there was a new, black Adventist church with a membership of around 400. Sometime in 1958 or 59, Little Richard came to town during his sojourn in the Adventist church and was the featured guest at the black church. My wife and I decided to go hear him. For some reason we were a minute or two late and the place was packed. But immediately a smartly dressed usher wearing immaculate white gloves approached us and ushered us down to seats in the front of the church. Why? What was so special about us? I wasn’t wearing a uniform. We were just a young couple with no VIP markers. Except white skin. It made me distinctly uncomfortable. Especially since the black choir, when guests of the white church, was required to enter via the back stairs into the church rather than the front entry.
In those presegregation days, restrooms were always “Men,” “Women,” and “Colored.” And, of course, the “Colored” were always consigned to the back of the bus.
My job was as a “toxicologist” at CDC’s Technical Development Laboratory on Oatland Island. The building was originally constructed as a retirement home for railway workers. Later it was acquired by the government to be used as a rapid treatment center for syphilis. After the arrival of penicillin, it was turned into TDL. As if the swampy southern east coast didn’t raise enough mosquitoes in the great outdoors, TDL raised millions more in its own mosquito vivarium. The purpose was to study the biology of different species. This was undoubtedly an improvement of my observation that whenever I patted one on the back it left a red splotch as a reminder of why I observed that mosquitoes suck.
So, after all this rambling, let’s get back to is my bottom-line assessment of the Tuskegee Syphilis Study. This is how this one observer sees it:
In 1932 the study was reasonable and justifiable given the current state of knowledge about syphilis.
The study was flawed from the beginning because the participants were treated with arsenicals although in a suboptimal dosage.
When penicillin became widely available and accepted circa 1950, the youngest subjects were at least in their forties and it was unclear whether treatment would significantly alter their health status.
In 1957 (when I was at CDC), it was deemed advisable to continue the study because there was much more to be discovered. But by then it was a bit like holding a tiger by the tail.
The participants were generally well treated, if Nurse Rivers story is to be believed. And I believe her.
But it is true that the participants were treated as guinea pigs in the sense that they did not give “informed consent.” But how does one “inform” uneducated sharecroppers?
The study helped result in more stringent ethical guidelines – as it should have – but it is unfair to retroactively apply those guidelines.
Others may disagree (and have) but these are my tentative conclusions. What think you?
P.S.: The best definitive study is “Bad Blood. The Tuskegee Syphilis Experiment” by James H. Jones. (1993)
Gordon Short, MD
Brevis Corporation